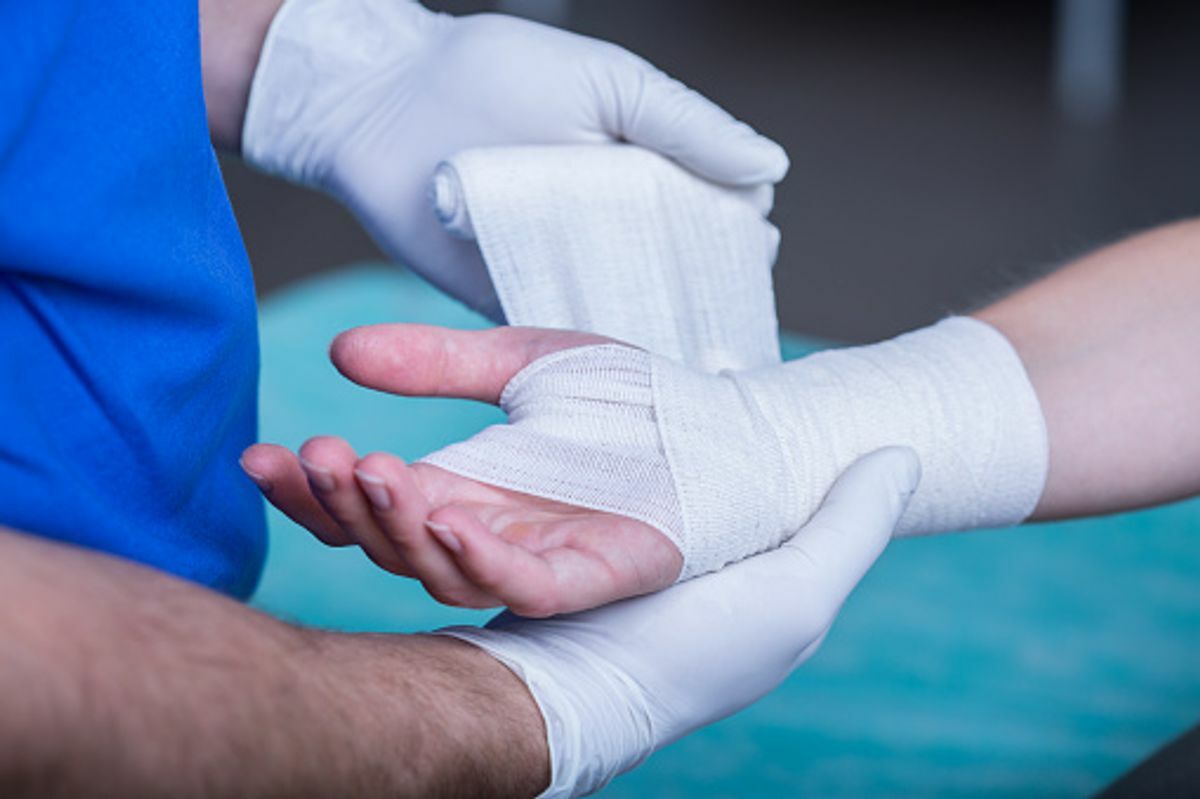
Old habits die difficult. Sometimes we do points a certain way simply because it does not take the way it has always been carried out. This is true even in medicine. We sometimes get stuck in a mentality of practicing a certain method through habit and no other reason. Best way to find the wound care in Fresno.
Wound care is not an exception. Many healthcare experts continue to treat and gown wounds the way it has been low years, even though new investigation shows this may not be the best therapy modality for the patient.
This post will examine three common misconceptions in wound care that have been found to delay injury healing, increase patient pain, and place a person and your employer at risk of negligence.
Betadine and peroxide help wound healing by reducing the bacteria within the wound bed. This has been a typical practice in treating chronic wounds for many years; however, it is no more acceptable practice, and carrying on to use these agents (and other similar agents) is harmful instead of helpful. Typically the Agency for Health Care Study and Policy (2008) claims,
Do not use povidone-iodine, iodophor, sodium hypochlorite, hydrogen peroxide, and lactic acid as cytotoxic. Use normal saline at the pressure between 4 along with 15 pounds per sq inch (psi). Using cytotoxic agents to cleanse chronic wounds can increase your patient’s distress, and delay wound therapeutic.
Dallam et al. (2004) reiterate this point: “Do not necessarily use cytotoxic solutions, for instance, Betadine or hydrogen peroxide, to cleanse wounds. That they not only deter wound therapeutic, but they may also cause using up and cold to sufferer discomfort.
Gauze dressings are an effective and cost-efficient approach to promote wound healing. Ovington (2001) states that for gauze dressings to provide the best recovery, they must be altered frequently or, at the very least, pre-moistened frequently.
This is labor-intensive, intended for health care practitioners or caregivers, and not cost-effective in today’s medical climate. Most importantly, gauze dressings do not support optimal hurt healing.
Ovington points out how the use of wet-to-dry dressings is not acceptable, as the debridement with this method of administration is not selective, often eliminating healthy tissue and leading to reinjury to the wound mattress, not to mention additional pain for your patient.
Frequent dressing modifications with gauze dressings will certainly reduce wound infections. New research has shown that bacteria can handle penetrating up to 64 levels of dry gauze, therefore negating the idea that gauze offers an effective barrier to germs.
Frequent dressing changes provide more opportunities for germs to enter the wound. Additionally, the labor associated with 2-3 times a day outfitting changes is not feasible most of the time. The practices mentioned are harmful to the patient, causing postponed wound healing and improved pain, but are also a legal responsibility risk for the practitioner and agency.
They use these types of methods of wound management. They may be no longer considered the best exercise and are no longer the standard associated with care.
In these days of quick change and a surge in new research and knowledge, how can practitioners be anticipated to keep up with new standards associated with care? Online learning with WoundEducators. Com is one process that can help you stay current while using new guidelines and the comfort of knowing that supports them.
We are devoted to ensuring that practitioners have almost all the up-to-date information they need to deal with wounds in their patients and effectively.
Read Also: Advantages Audiologists – Read Now